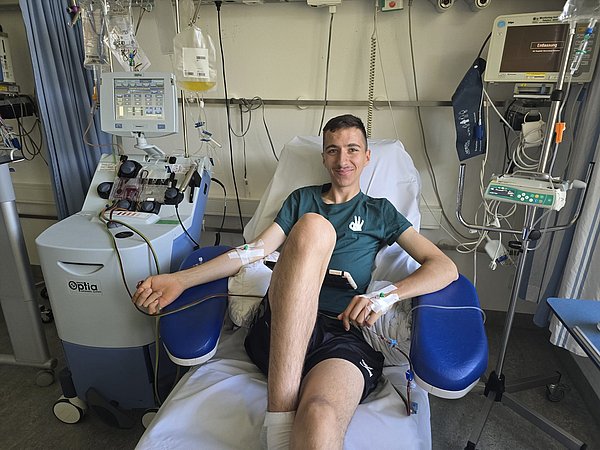
No further treatment available. That was the diagnosis in early 2025. Mailo, then 17 years old, had been battling cancer for ten years. When he was seven, a harmless-looking lump turned out to be a malignant kidney tumor. The tumor was surgically removed, followed by chemotherapy. Two years later, the first metastases were discovered. From then on, the cancer continued to spread. In the end, tumors were found on his liver and spleen, on his lungs, and in his brain. “I wondered whether it was ethically acceptable to give him hope at this point,” recalls Christian Seitz. He is a senior physician and medical director of cell and gene therapy at KiTZ. However, when physicians and scientists took a closer look at Mailo's tumor cells, they discovered that all the cancer cells produced a specific protein molecule called PRAME. This was good news.
This opened up the possibility of immune cell therapy. “The idea is to activate the body's own immune system against the tumor cells,” explains Seitz. There are various methods of getting the immune system to fight cancer. In Mailo's case, the immune system's defense cells, the T cells, were to be genetically modified so that they recognize tumor cells and attack them specifically. Genetic modification means that, by using a virus, a genetic blueprint is introduced into the cells, which are first extracted from the patient's blood. Based on this blueprint, a receptor is created on the T cells that is programmed to recognize the specific protein molecules of the tumor – in this case, the PRAME protein. This enables the T cells to recognize and kill the tumor cells.
In order for KiTZ to be able to carry out such a treatment, it needs approval from the relevant authorities for an individual therapeutic trial. Although immunotherapies have been around for several years, they are used almost exclusively in adult cancer patients. In children, these forms of therapy are relatively new and are mainly used only for a specific form of blood cancer.
On July 2, 2025, Mailo received the modified immune cells via infusion. He is in intensive care because there is a high risk that his immune system will go haywire when the T cells launch their attack. Three days later, Mailo develops a high fever. “This is when the programmed T cells multiply explosively,” explains Seitz. According to Seitz, 120 days later, there is no longer any living tumor tissue detectable; no tumor cells can be found in the blood either. “Objectively speaking, this was not to be expected,” says the physician-scientist. He would have been thrilled if the many small tumors on the organs had been eliminated. “We would then have operated on the larger tumors in the spleen, liver, and lungs.”
But Mailo's goal was always clear: “I wanted to get back on my bike.” He has already participated in several downhill biking competitions and says that this has given him strength and joie de vivre. Now he wants to continue cycling. And he wants to catch up on his high school diploma because, “I want to study medicine in Heidelberg and then become a doctor.”
Meanwhile, preparations are underway at KiTZ for a clinical trial that aims to prove that Mailo's case was not an isolated one, but that this type of immunotherapy also works in children and adolescents. Fifteen to eighteen young cancer patients are to be included in the study. Seitz is urging swift action, as treatment options specifically for children with cancer after a relapse are limited. “These children cannot wait; they need new, effective therapies.”
Source: Stefanie Ball